Data Speaks: What Early Adopters Are Seeing
Evidence from leading cancer centers confirms that integrating AI into radiation oncology is not theoretical—it’s transformative. Institutions that have successfully embedded AI into their workflows are already reporting:
- Increased throughput without expanding staff
- Improved consistency across physicians and treatment sites
- Enhanced precision in treatment planning and delivery
- Greater physician satisfaction as repetitive tasks are automated
- Better patient outcomes through more accurate, timely interventions
Crucially, these benefits accrue to clinicians who embrace AI—not those replaced by it. The data supports a simple truth: AI enhances practitioners who choose to work with it.
The Strategic Imperative: Adaptation or Obsolescence
That Harvard instructor’s warning—“Physicians who don’t adopt AI will be left behind”—isn’t alarmist. It’s market reality.
As AI-enabled peers deliver faster, more consistent, and more accurate care, traditional practitioners face pressure from multiple fronts:
- Institutional expectations for greater efficiency and measurable outcomes
- Patient demand for providers using cutting-edge technologies
- Economic competition from practices with superior AI-driven productivity
- Evolving professional standards that increasingly expect AI literacy
In short: AI adoption is no longer optional. It’s a strategic imperative for staying relevant and competitive in modern healthcare.
Addressing Implementation Barriers
Recognizing the importance of AI is one thing—successfully implementing it is another. Clinicians often cite four main barriers:
- Technical Overwhelm: The belief that AI mastery requires coding or data science skills.
- Integration Anxiety: Fear that AI will disrupt established workflows.
- Trust Deficits: Uncertainty about when to rely on AI versus human judgment.
- Financial Concerns: Doubts about cost, ROI, and sustainability.
The key insight: successful AI adoption doesn’t demand clinicians become data scientists—it requires they become strategic partners in AI integration.
The Path Forward: Partnership, Not Replacement
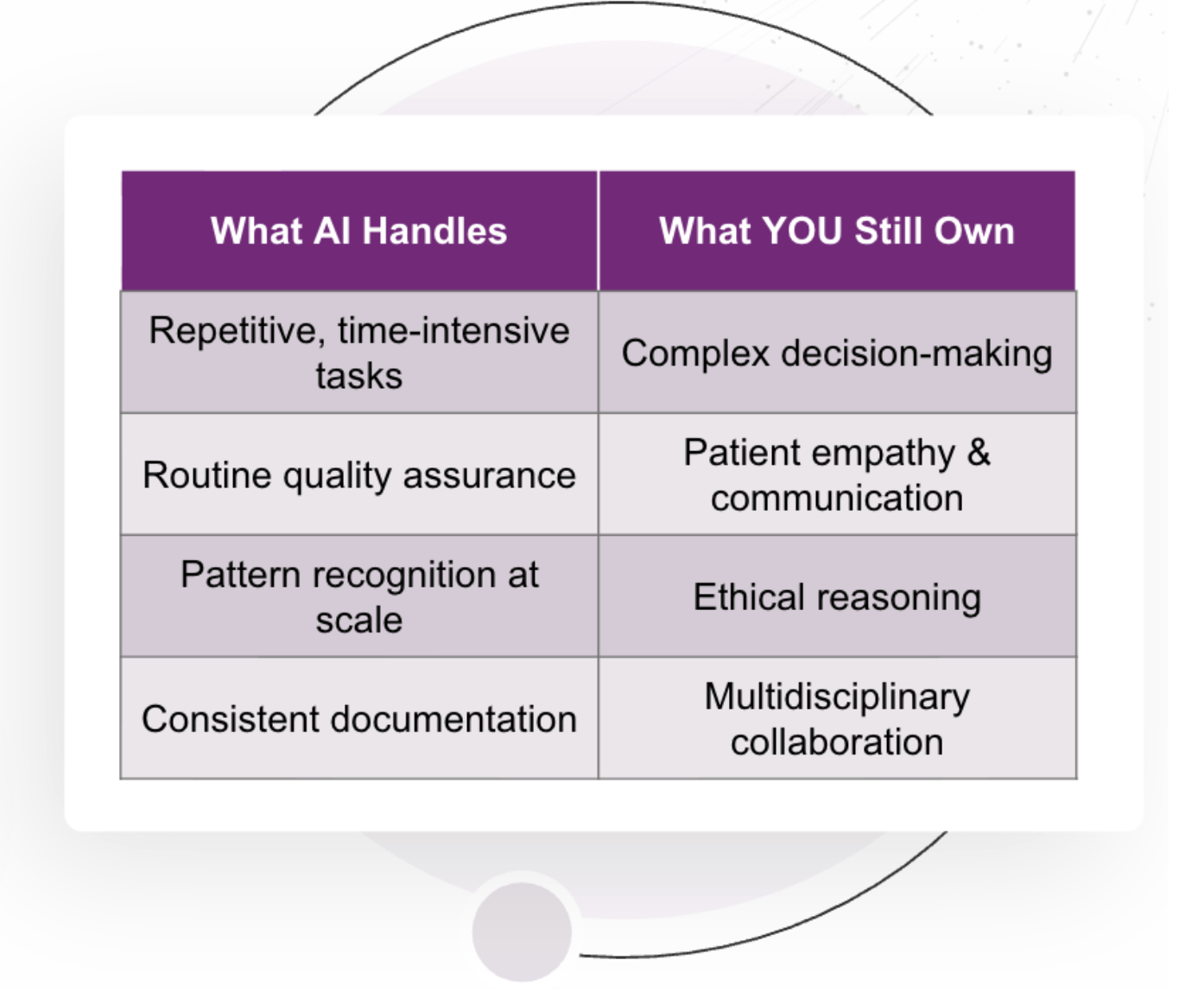
The most effective AI programs in healthcare follow a partnership model, where technology augments, not overrides, clinical expertise. These models share several defining features:
- Clinicians retain decision authority, using AI as an advisor.
- Seamless workflow integration, making AI feel like a natural extension of daily practice.
- Continuous learning loops, enabling both humans and machines to improve over time.
- Human oversight, ensuring accountability and managing edge cases.
This approach explains why MedLever’s workflow-embedded systems resonate with forward-thinking oncology groups. Instead of forcing clinicians to adapt to AI, these tools adapt to clinical workflows—creating enhancement without disruption.
Embracing Enhancement Over Replacement
The question “Will AI take my job?” belongs to yesterday’s mindset. Tomorrow’s opportunity lies in augmentation, not replacement.
The physicians thriving in AI-enhanced environments aren’t those who resisted automation—they’re the ones who led the integration. They understand that the future of medicine belongs not to artificial intelligence or human intelligence alone, but to the synergy between the two.
For radiation oncologists, the choice is clear: Lead AI integration within your specialty—or watch others define it for you.
Technology will advance with or without your participation, but your competitive position, professional fulfillment, and patient impact depend entirely on which side of that adoption curve you choose.
Key Takeaway
AI isn’t the end of the physician’s role—it’s the evolution of it. Clinicians who partner with AI aren’t being replaced; they’re being amplified.
Authored By: Padmasri Bhetanabhotla